TAINAN, Taiwan, Aug. 3, 2022 /PRNewswire/ — When the body’s immune system turns on itself and attacks the body’s healthy cells and organs, we develop autoimmune disorders. A rare entrant in the list of autoimmune disorders is acquired hemophilia A (AHA) in which spontaneous bleeding occurs in patients with no previous history of the condition. Although AHA is often associated with significant mortality, owing to its rarity, there is very little data on the underlying physiological processes.
Are other diseases that involve considerable immune suppression, for instance viral infections, associated with AHA? A group of researchers led by Dr. Ya Ting Hsu and Dr. Peng Chan Lin of the NCKU Hospital, Taiwan, have recently reported a case that points towards such a possibility.
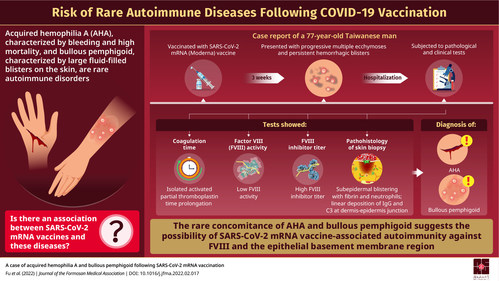
In their case report published in the Journal of the Formosan Medical Association, the researchers detail the symptoms, diagnosis, and treatment of a 77-year-old Taiwanese man who presented with bruised-looking skin on his forearms and legs along with bleeding blisters on his hands and trunks three weeks after receiving the second dose of the mRNA Moderna vaccine against the viral infection, COVID-19. Pathological and clinical tests, including blood coagulation factor VIII (FVIII) titer and FVIII inhibitor level estimation, and a skin biopsy confirmed AHA concomitantly occurring with bullous pemphigoid, a rare autoimmune skin disease. "The simultaneous diagnosis of AHA and bullous pemphigoid is very rare. Multiple studies have indicated that medications or vaccines play a role in inducing bullous pemphigoid, but the progression to this condition is still unclear. Although the causality and pathogenesis of the autoimmune conditions in our patient remains unconfirmed, we reported this case to raise awareness of this rare phenomenon following SARS-CoV-2 mRNA vaccine administration," explains Dr. Hsu.
mRNA vaccines are till date the first line of defense against SARS-CoV-2-induced COVID-19. Awareness of autoimmune diseases associated with these vaccines can help physicians provide timely treatment and prevent significant morbidity and mortality in patients. "There are several questions that need to be asked if we are to understand vaccine-related autoimmune diseases. For example, do patients with known autoimmune diseases have a higher risk of developing vaccine-related autoimmune disease? Can they receive a SARS-CoV-2 mRNA vaccine safely? Will the vaccine trigger flare up of an existing autoimmune disease? Will these patients be treated differently?" observes Dr. Lin, while explaining the need for extensive, timely, and honest reporting of relevant incidents.
Besides reporting their case, the researchers studied existing literature and identified six other vaccine-related cases of AHA reported since 2021. They found that all six patients were administered with either Moderna or Pfizer-BioNTech vaccine and that treatment took less time in all cases than in non-vaccine associated AHA. Apart from the six COVID-19 vaccination-related cases, two more AHA cases following influenza vaccination, which uses a different antigen, were also reported. The researchers suggest that if more autoimmune diseases following SARS-CoV-2 mRNA vaccine administration are reported, further investigation into their pathogenesis can be made, which can then help identify the potential at-risk groups.
These findings point to a possible association between SARS-CoV-2 mRNA vaccines and autoimmune diseases like AHA. Further studies are needed to conclusively prove a causal link between the two. Through timely reporting of such cases, the short-term and long-term side effects of mRNA vaccines against COVID-19 can be better understood and patient management improved for better outcomes.
Reference
Title of original paper: A case of acquired hemophilia A and bullous pemphigoid following SARS-CoV-2 mRNA vaccination
Journal: Journal of the Formosan Medical Association
DOI: https://doi.org/10.1016/j.jfma.2022.02.017
Contact:
Yu-Ting Chen
+886 6 2757575 ext. 80921
341812@email4pr.com
SOURCE National Cheng Kung University